Shopping for health insurance can be a confusing endeavor. Not only does a consumer have to keep up with the changing health care laws, but they also have to understand health insurance terminology, how premiums and deductibles work and be able to select a plan that suits their needs while still keeping within their budget. None of that is easy. That’s where decision support tools come in. When you operate a State-Based Marketplace, you have the freedom to decide what types of tools you want to offer to your residents—it’s one of the many perks of having your own state exchange.
GetInsured has been a leader in decision support technology that simplifies the health insurance enrollment process. We can define insurance terminology each step of the way, rank plans based on stated consumer needs instead of just ranking in order of monthly premium, and include prescription drug and provider search to determine best plan coverage. GetInsured decision support tools are currently being used by millions of consumers in states such as California, Minnesota, Washington, and launching this year, in Nevada.
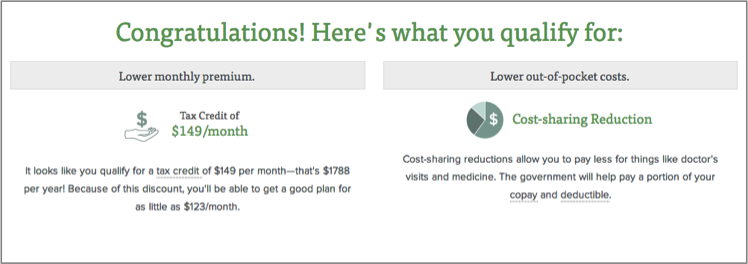
Eligibility and Tax Penalty Calculator: Customers can instantly determine their eligibility for money-saving tax credits with the GetInsured calculator, which is 99.9% accurate and was recognized by Consumer Reports as best in class. Our calculator is unique in that it can handle households with complex scenarios, where family members may qualify for various programs. If the customer’s eligibility check determines he/she is eligible for Medicaid/CHIP, our system immediately redirects the customer to the state’s Medicaid/CHIP website/call center.
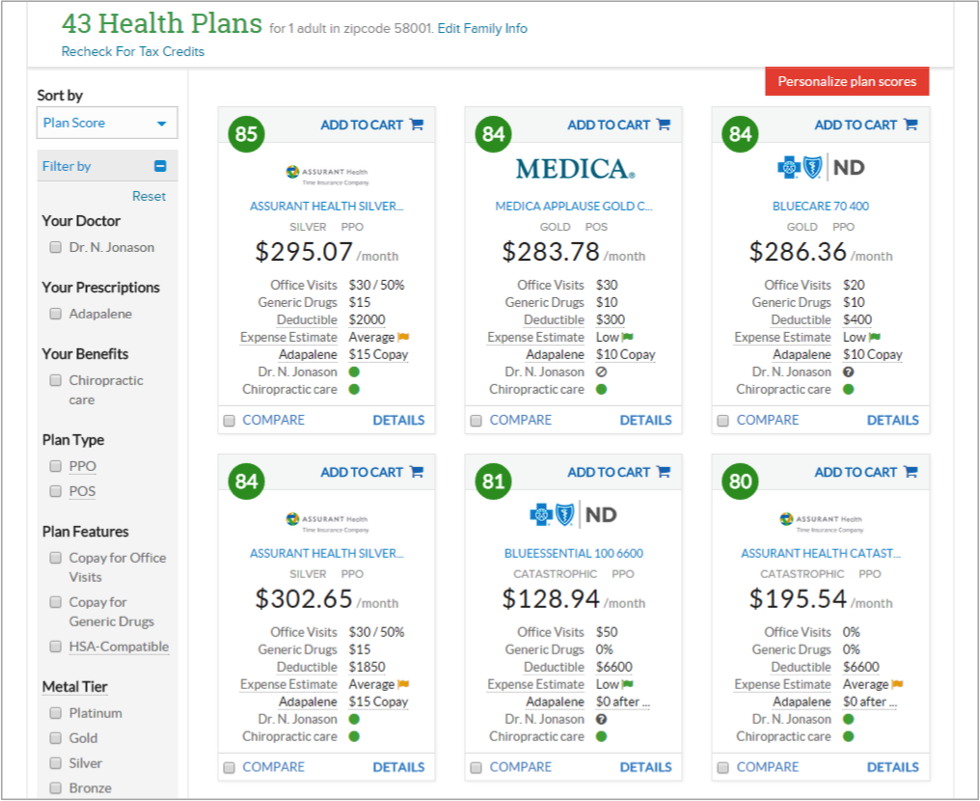
Plan Shopping: GetInsured uses its proprietary plan ranking technology, the GetInsured Plan Score (GPS), to present customers with a sorted and scored list of plans that are the most cost-effective for the projected usage pattern. GPS empowers consumers to choose plans based on estimated total out-of-pocket expenses versus choosing a plan based solely on the lowest monthly premium amount.
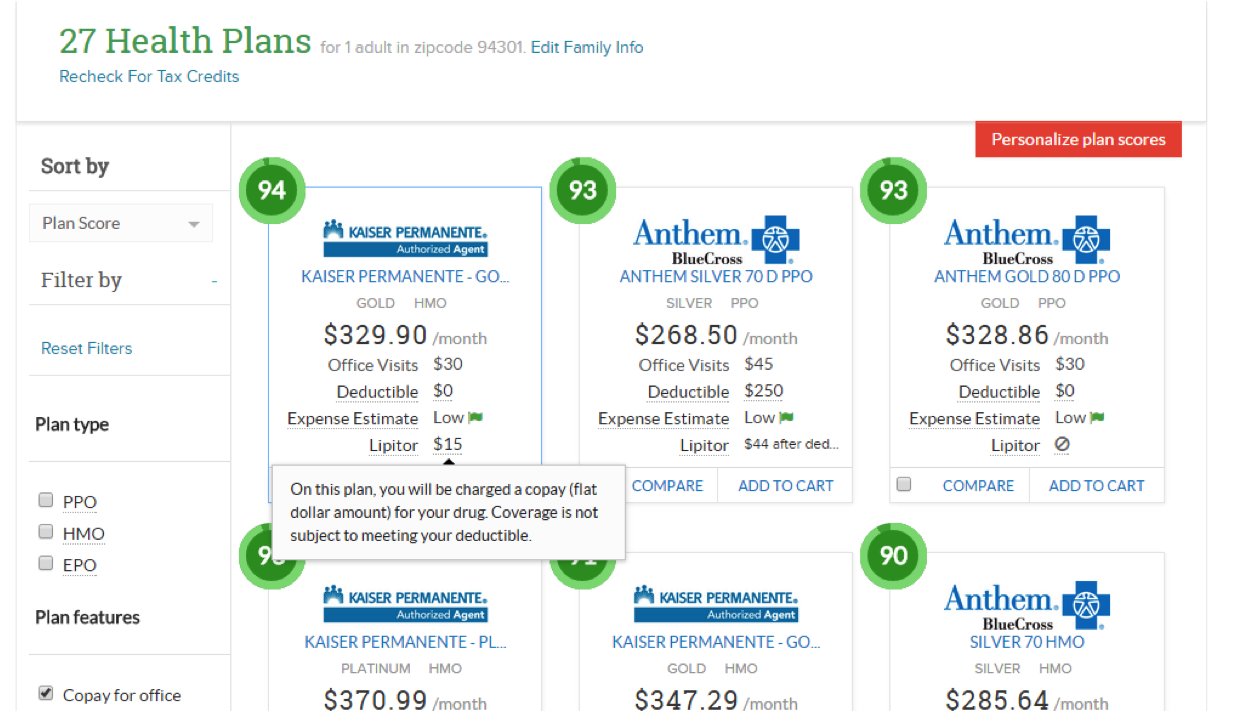
Provider Networks and Prescription Drug Search: Customers can search for plans that include their preferred doctors and prescription drugs, see doctors in the plan’s network within a 10-mile radius plotted on a map, and instantly access detailed plan data, including the list of providers who accept the plan.
Want to learn more about how these—and other—tools can help shoppers in your state? Email our Business Development team at hello@getinsured.com.






